What does a behaviour support practitioner do? A Q&A with Cairns PBS practitioner, Laya Brown

No idea what a behaviour support practitioner actually does? We’re here to answer the question many people are asking, “What does a behaviour support practitioner actually do?”.
Do they support behaviour? Change behaviour? Perhaps they analyse behaviour? Let’s find out with Laya Brown, a behaviour support practitioner in Cairns, Far North Queensland.
What does a behaviour support practitioner do?
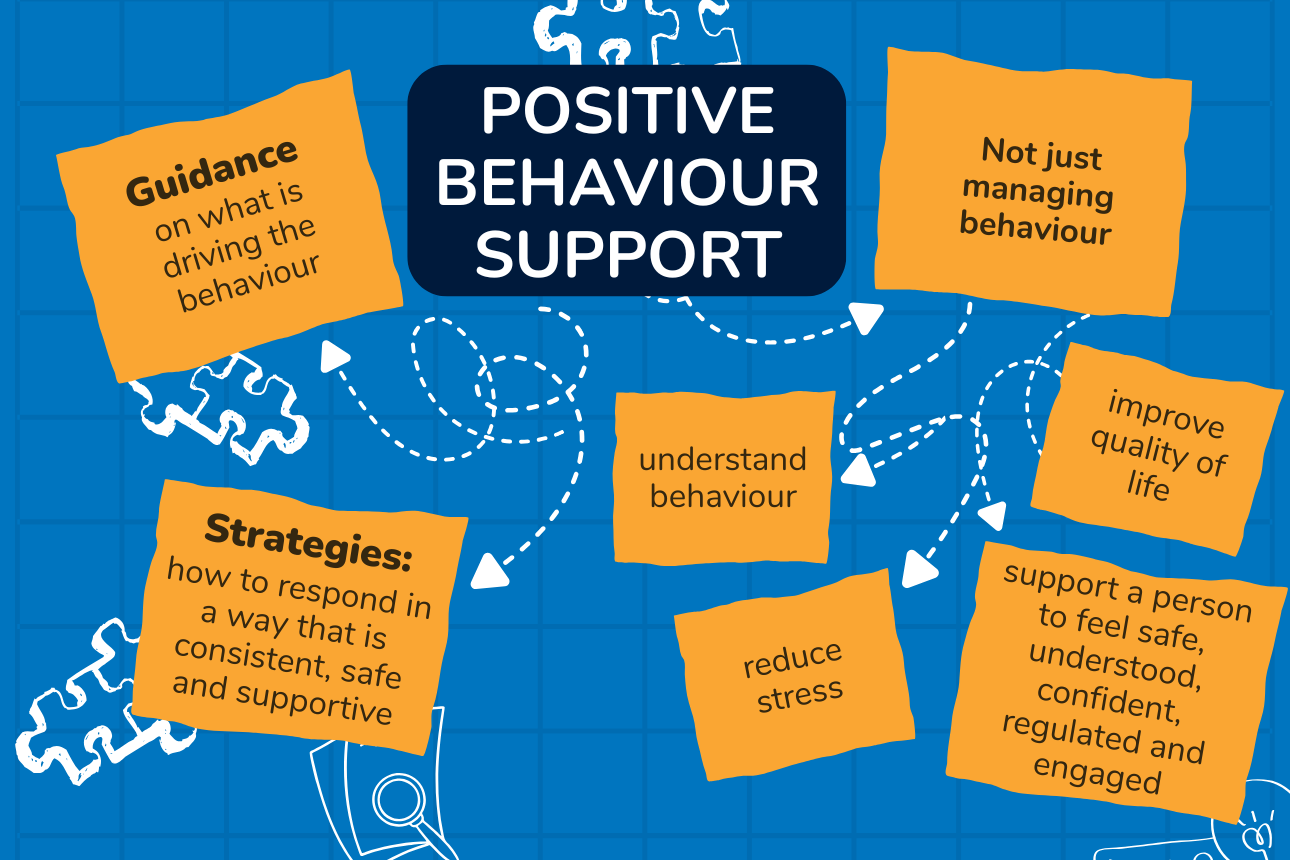
A behaviour support practitioner works alongside a person, their family, and their support team to understand what might be driving certain behaviours and how we can better support them to improve their quality of life.
It’s not about fixing or changing the person, but rather looking at their environment, communication, and needs, to understand why the behaviour is occurring.
From there, we identify what supports are needed and implement practical strategies to help reduce or prevent those behaviours. Once we have a clear understanding, we focus on improving quality of life, reducing stress, and supporting the person to feel safe, understood, and more in control.
Why do people look for help from a behaviour support practitioner?
People usually look for help from a behaviour support practitioner when something isn’t working and they need a better understanding of how to support the person in a way that actually improves their quality of life. This can be through referrals from families, support teams, or professionals, and people can also refer themselves if they feel they need support. This might be when behaviours of concern are occurring, such as aggression, withdrawal, emotional distress, or difficulties with communication.
For example, this could look like a child struggling at school and becoming overwhelmed, someone becoming upset or aggressive when their routine changes, or a person withdrawing and not engaging in daily activities. It can also be situations where a person is using behaviours to communicate a need, but it’s not being understood by those around them.
Often, families and support teams are doing their best but need guidance on what’s driving the behaviour and how to respond in a way that is consistent, safe, and supportive in the long-term. The goal is not just to manage behaviour, but to understand it, reduce stress, and support the person to feel more confident, regulated, and engaged in their day-to-day life.
When you first start working with a participant, what do you do first and why?
The first thing I focus on is building rapport and getting to know the person properly. That means spending time with them, talking to their supports, and understanding their routine, preferences, and what their day-to-day life looks like. I also gather information from the people around them to get a full picture. This is really important because you can’t support someone without understanding them first.
What can participants expect from their behaviour support practitioner after their first meeting/discussion?
After the first meeting, participants can expect ongoing, tailored support that is built around their individual needs and goals. This is a collaborative process, where I work closely with the participant, their family, and support team to put practical strategies in place and make meaningful changes over time.
From there, support typically includes:
- Developing a personalised behaviour support plan
- Providing practical strategies that can be used day-to-day
- Training and collaborating with families, allied health, schools, carers, and support workers
- Regular check-ins to review what’s working and what needs adjusting
- Supporting skill development and building independence over time.
How long does it take before NDIS participants receive practical advice or strategies they can apply?
In most cases, participants and their support team can start receiving practical strategies quite early on. While we are still getting to know the person, we can often suggest simple, immediate strategies that can be trialled straight away.
As we gather more information and build a clearer understanding, those strategies become more tailored and effective over time. It’s an ongoing process, but the goal is to provide support that is useful from the beginning, not just at the end.
What if restrictive practices are being used — what is your role in these situations?
If restrictive practices are being used, my role is to work collaboratively with the participant, their family, carers, and support team to make sure everything is understood, appropriately documented, and only used when absolutely necessary and in line with legislation. I also help the team understand why the behaviour may be occurring and what proactive strategies can be put in place to reduce risk and better support the person.
A big part of my role is supporting everyone around the participant, so carers and support workers feel confident, informed, and supported in how they respond. The overall goal is always to reduce and, where possible, eliminate restrictive practices over time by building safer, more positive, and more effective supports.

Will participants always need their behaviour support practitioner?
Not always, the aim of behaviour support is to build the capacity of the participant and the people around them, so over time they feel more confident and supported without needing ongoing input from a practitioner. We regularly review and reassess supports to make sure they are still needed and effective. As things improve, involvement can reduce, and ideally, the person and their team feel equipped to manage things independently.
How do NDIS participants get started with Positive Behaviour Support?
Make an online referral for Positive Behaviour Support on our website. You are also welcome to contact us if you have any questions about PBS, on 1300 694 625 or by using our contact form.
About Laya Brown, Behaviour Support Practitioner in Cairns
Laya, tell us about you!
Hi, I’m Laya! I’m a Behaviour Support Practitioner based in Cairns, Far North Queensland. I’ve been working in the disability sector for over five years, and my passion for this work really started during a placement at Hands on SA in Adelaide, where I supported individuals with disabilities in employment. That experience stayed with me and shaped the direction I wanted to go in.
After moving to Cairns, I worked in employment services helping people with disabilities gain and maintain meaningful work, before transitioning into disability support. This gave me a really hands-on understanding of what day-to-day life can look like and the importance of the right supports being in place.
What I love most about this role is building genuine connections with people and being able to support them in a way that actually makes a difference. I’m really passionate about helping people feel heard, understood, and supported, and working alongside families and support teams to create positive, meaningful outcomes. 
What drew you to the field of Positive Behaviour Support?
Working as a support worker, I saw first-hand how often behaviours were misunderstood or responded to in ways that didn’t actually help the person long-term. A big turning point for me was supporting a client with Huntington’s disease, where I saw a sudden change in behaviours after knowing him for so long. It really made me step back and look at things through a behaviour support lens, trying to understand what was actually driving those changes rather than just reacting to them.
During that time, I worked closely with my team leader, who was also the client’s Behaviour Support Practitioner, and she was the one who really planted the seed for me to move into this field. That experience stuck with me, and it ultimately led me to pursue Positive Behaviour Support, a space where I could focus on understanding the “why” behind behaviour and creating more meaningful, long-term change.
What have you learnt from working in the disability sector that influences your work as a behaviour support practitioner?
One of the biggest things I’ve learnt is that behaviour is always communication, even when it doesn’t look like it on the surface. A lot of the time, people aren’t being “challenging” they’re trying to express a need that isn’t being met, and it’s our job to understand what that is.
I’ve also learnt how important consistency is across teams, and how much of a difference it makes when everyone is on the same page. A big part of that is working closely and collaboratively with the main support worker, as they often know the person best and have the most day-to-day insight.
Building strong relationships is key, once trust is there, everything else becomes a lot easier. Taking the time to really get to know the person, their preferences, and what matters to them makes a huge difference in outcomes.
I’ve also learnt that small, practical changes can have a really big impact. It doesn’t always have to be complex, sometimes it’s about adjusting the environment, communication, or routine in a way that better supports the person.
Overall, these experiences have shaped my approach to be patient, collaborative, and focused on long-term, meaningful change rather than quick fixes.

How would you describe Positive Behaviour Support to someone who has never heard of it?
Positive Behaviour Support is about understanding the “why” behind behaviour and supporting people with positive, practical strategies that improve their quality of life, not just trying to stop the behaviour itself.
Can you share an example of how Positive Behaviour Support can help a person improve their quality of life?
One example that really stands out to me was supporting a client with Huntington’s disease, where over time he lost the ability to clearly communicate his thoughts and needs. Because of this, behaviours became one of the main ways he was expressing himself.
I remember there were incidents occurring during showering, so instead of just responding to the behaviour, I took a step back and asked, “What is actually going on here?” I spent time researching his condition to better understand how he may be feeling, and I really tried to put myself in his shoes. I even sat on his shower chair and thought, if I was in his position, would I feel safe and comfortable? The answer was no.
From there, I brought in an OT to assess the environment and worked closely with the team to adjust how we were supporting him. Once changes were made, we saw a reduction in distress and a much more positive experience for him.
This really reinforced for me that when we take the time to understand the person and their environment, and work collaboratively as a team, we can make meaningful changes that significantly improve someone’s quality of life.
Do you support NDIS participants in any specific age groups or with certain disabilities?
I support a range of participants across different age groups, including children, adolescents, and adults. I have experience working with individuals with autism, ADHD, psychosocial disabilities, and intellectual disabilities, as well as those presenting with complex behaviours of concern.
I take a very individualised approach, as no two people are the same, and I work closely with each person and their support network to understand their needs and provide tailored support.
To get started with Positive Behaviour Support in Cairns, please feel welcome to make a referral for Positive Behaviour Support anytime.

Being in Far North Queensland, you probably have a few considerations that other behaviour support practitioners don’t need to worry about.
Working across Far North Queensland comes with unique considerations, particularly in relation to distance, travel time, and access to services, as Cairns and surrounding areas are quite spread out. Some participants reside in more remote locations, which can make consistent access to supports more challenging.
I aim to make this as seamless as possible for participants, families, and support teams by being flexible in how services are delivered. I am able to travel to a range of locations where required, including areas involving extended travel, and I also utilise telePBS, where appropriate, to maintain continuity of support.
My goal is to ensure services remain accessible and consistent, so participants and their families do not have to manage the added stress of logistics, and can instead focus on receiving the support they need.
Where do you provide Positive Behaviour Support in Cairns?
Our team supports NDIS participants with person-centred Positive Behaviour Support in Cairns and surrounding areas, including travel from Tully to Mossman/Daintree and across to the Atherton Tablelands, including, but not limited to:
Central/Inner Cairns
- Cairns City (CBD)
- Cairns North, Parramatta Park, Bungalow, Portsmith, Westcourt
- Edge Hill, Whitfield, Kanimbla, Manoora, Manunda, Mooroobool, Earlville, Woree, Bayview Heights, Aeroglen
Northern Beaches and northside
- Machans Beach, Holloways Beach, Yorkeys Knob
- Smithfield, Trinity Park, Trinity Beach, Kewarra Beach, Clifton Beach, Palm Cove, Ellis Beach
Redlynch / Freshwater Valley
- Freshwater, Stratford, Brinsmead, Redlynch, Caravonica, Kamerunga
Get started with Positive Behaviour Support in Cairns
Make a referral for Positive Behaviour Support on our website. You can do this anytime and you can make your own referral, or a member of your support team can make a referral on your behalf.
If you have any questions about Positive Behaviour Support, please feel welcome to call our team on 1300 694 625 or send a message using our contact form.
Contributors
Written by Laya Brown, Behaviour Support Practitioner, Cairns
Laya is a Behaviour Support Practitioner based in Cairns, with over five years’ experience in the disability sector. She takes a warm, down-to-earth approach and values building genuine connections with the people she supports. Laya is passionate about helping individuals feel heard, understood, and supported to create meaningful improvements in their quality of life.
Reviewed by Indi Taylor PGDipPsych (JCU), BA/BEd (SCU), AdvDipCSC, Cert IV TAE, Senior Behaviour Support Practitioner and Team Leader, Cairns
Indi’s practice is grounded in person-centred, trauma-informed, and strengths-based approaches. She works with adults with complex presentations including ASD, psychosocial disability, neurodegenerative conditions, and post-stroke support, with a strong focus on dignity, freedom, capacity, and risk.